MRgFUS (Magnetic Resonance Guided Focus
Ultrasound) uses MRI and ultrasound to find your
fibroids and then to apply ultrasound-generated
energy to heat the fibroids up in order to destroy
them.
This is not a surgical procedure and does not
involve cuts or incisions. It is typically performed
by an interventional radiologist.
This procedure aims to relieve abdominal pain
and cramping, heavy menstrual bleeding,
anaemia, distended stomachs, and constipation,
which are caused by fibroids. Fibroid volume
may be shrunk by 30 ± 24 % after 4 months.
Other alternatives for relief of symptoms caused
by fibroids include:
- For heavy menstrual bleeding: non-hormonal
oral medications, or hormonal oral
medications, or a hormonal coil (e.g. Mirena)
or
- For bulk-related symptoms in addition to
heavy bleeding: (i) minimum invasive
procedure such as transcervical resection of
fibroids (TCRF) or uterine artery embolisation
(UAE/UFE), or (ii) extensive surgery such as
abdominal myomectomy, or (iii) a long-term
permanent solution of hysterectomy.
MRgFUS is only suitable for small fibroids
(larger than 3 cm and less than 10 cm) of
average size less than 7 cm where the high
intensity ultrasound energy does not pass
through the bowel or bladder on its way to
reach the fibroids.
Suitable fibroid types include:
- Submucosal that causes bleeding,
- Subserosal without narrow stalk that
causes pressure/urinary symptoms.
When is this procedure unsuitable?
MRgFUS is unsuitable when you have:
- Fibroids over 10 cm/500 mls.
- Obstructions in the treatment beam path
such as a scar (e.g. c-section), skin fold,
bowel, intrauterine device or any hard
implants;
- Fibroids that are close to sensitive organs
such as the bowel or bladder;
- MRI related issues such as an allergy to
contrast agent or metallic implants or
overweight;
- Pregnancy;
- IUD;
- Cardiac, cerebrovascular, bleeding,
haematological, neurological disorder or any
pelvic infection.
I have multiple fibroids, is it still
OK for me to have MRgFUS?
MRgFUS is not recommended for 6 or more
symptomatic fibroids.
Will I still be able to have children
afterwards?
There are only a handful of reports of pregnancy
(mainly in cases of single fibroid ablations),
currently, this procedure in NOT recommended
for women who still want children.
What are the risks or complications
of the procedure?
Risks and complications of MRgFUS are relatively
low and include:
- Possible skin burns.
- Pain &/or swelling in the treated area.
- Back or leg pain.
- Nerve damage.
- Nausea.
- Abdominal cramping.
- Fever.
- Vaginal discharge.
- Urinary tract infection.
- Bowel perforation.
What are pre-procedure
treatments?
You may be prescribed injectable hormone such
as GnRH analogues (e.g. Zoladex or
DecapeptylÂ) to reduce the size of the fibroids
to make the procedure easier. This is particularly
recommended for fibroids larger than 8 cm.
What happens at pre-assessment?
Pre-assessment usually takes place a week
before the actual procedure and lasts an hour. At
pre-assessment, certain tests are carried out to
make sure that you are fit for it, which include:
- Physical examination.
- Pregnancy test.
- Check what medications you are taking
regularly.
- Check blood pressure, heart rate and ECG
to see if the heart is fit.
What happens BEFORE the procedure?
- One week before: No aspirin or ibuprofen.
- On the day of treatment: you can continue
your normal medications, you may drink,
have light meal, but do not use talc, cream or
oil on the abdomen.
- All hair needs to be removed from the
umbilicus (belly button) to 1cm below the
pubic bone to prevent the formation of gas
bubbles which may cause burns.
- Any skin lotions must be removed with
alcohol as these may reduce the acoustic
coupling.
- You will be seen by the interventional
radiologist who will explain the procedure to
you, give you an opportunity to ask
questions and you will then be asked to sign
a written consent form.
What happens DURING procedure?
- A urinary catheter is connected to keep the
bladder empty during the course of the
treatment.
- Light sedation (usually titrated doses of
fentanyl and midazolam) is given to help you
relax, however, you will be conscious and
able to communicate with the interventional
radiologist during the whole procedure.
- You are required to lie on your stomach in
the MRI machine.
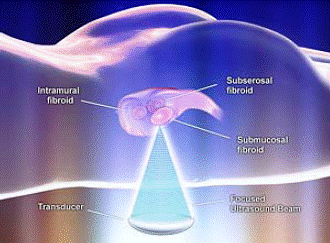
| Figure 1. The focussed ultrasound beam on uterine fibroids.
(Source: SightLine Houston) |
 |
- A dye is injected and the MRI will take images
of your fibroids, uterus and abdomen;
measuring size, shape.
- The ExAblate® 2000 System software uses
the pre-treatment MRI images to calculate
the number and type of sonications (doses of
focus ultrasound) required.
- Sound energy from each sonication is applied
directly to at specifically measured points to
produce heat up to 65-85 ºC which causes
the protein in the fibroid to become
denatured leading to eventual cell death.
Therefore, after each sonication, a small
volume of the fibroid is ablated (burnt away).
- Treatment typically consists of 20-50
separate sonications, lasting between 10-30
seconds each, followed by a 90 second
cooling period. Hence, after multiple
sonications the entire fibroid is ablated.
- The whole process takes up to 3-4 hours.
- Post-treatment imaging, before and after
administration of contrast agent, is
conducted immediately to calculate the
Âdying (necrotic) volume to assess how
effective the treatment is. The necrotic
fibroid tissue shows as non-enhancement on
the image.
What happens AFTER procedure?
- You will stay in hospital for up to two hours
after the treatment so that the hospital can
make sure you are well.
- After the treatment you may feel cramping
(similar to a menstrual pain), nausea and
soreness in the shoulders from lying flat. If
necessary, you may be given some light pain
relief medication.
- You will be given follow-up MRI
appointments at 4 and 12 months.
Going homeÂ
Â
You should be able to go home the same day.
Care at Home Guide
- After getting home, take it easy for the rest
of the day.
- You should be able to return to normal
activity or return to work in a few days.
- You may experience cramping symptoms. If
this is the case, you can take paracetamol
(e.g. Panadol) or ibuprofen such as Nurofen
(only if you are not allergic to it or asthmatic
or have history of stomach ulcer). If you are
in doubt, ask your pharmacist.
- If you experience any vaginal discharge or
have your first period soon after the
treatment, it is advisable that you use
sanitary towels for in order to reduce the risk
of infection.
- You should NOT have sexual intercourse for
at least one week, preferably 2 weeks.
- It is advisable to use condoms or a
diaphragm for at least 4 weeks if you are
sexually active.
When should I seek emergency
medical attention?
While it is unusual to have problem once you are
at home, seek immediate medical attention if
you develop heavy bleeding, severe abdominal
pain that is not relieved by pain killers or high
fever.
How do I obtain MRgFUS service?
In the UK, this treatment
method is not yet available on
the NHS. There have been a
few cases of sponsored
treatments by some PCTs
(Primary Care Trust) but your
GP has to make a case for it.
MRgFUS is available privately.
How much does it cost?
It costs between £4K and £5K
Where are the treatment centres?
Currently only one centre in UK is offering MRgFUS:
MR Therapy Centre- a private unit located
inside St. Marys Hospital (Paddington,
London).
What is the recurrence rate?
Because MRgFUS is a relatively new procedure,
the available data is limited to 2 years after
procedure (see Table 1).
| Table 1. Recurrence rates following MRgFUS |
| Follow-up period |
Rate (%) |
| 0 to 6 months |
0.80 |
| 6 to 12 months |
6.49 |
| 12 to 24 months |
3.63 |
| [Source: BJOG. 2008 April 1; 115(5): 653-662] |
There is a claim of 5 % recurrence rate of
MRgFUS compared with a higher rate for UAE and
myomectomy. It is worth pointing out that data
may be skewed because, firstly, MRgFUS is very
selective in the types, size and number of
fibroids being treated and secondly, the number
of patients being exposed to MRgFUS technique
is much less when compared to UAE/UFE or
myomectomy.
Can I have a repeat MRgFUS if it
was not so satisfactory first time?
If necessary, according to the commercial
protocol, a second session of MRgFUS can be
carried out within 2 weeks of the initial
procedure.
What are other alternatives
following MRgFUS?
When MRgFUS did not work at all, many consider
UAE/UFE or myomectomy as the next step and
failing all that is hysterectomy.
 Woman2Woman Fibroid Support
Woman2Woman Fibroid Support



