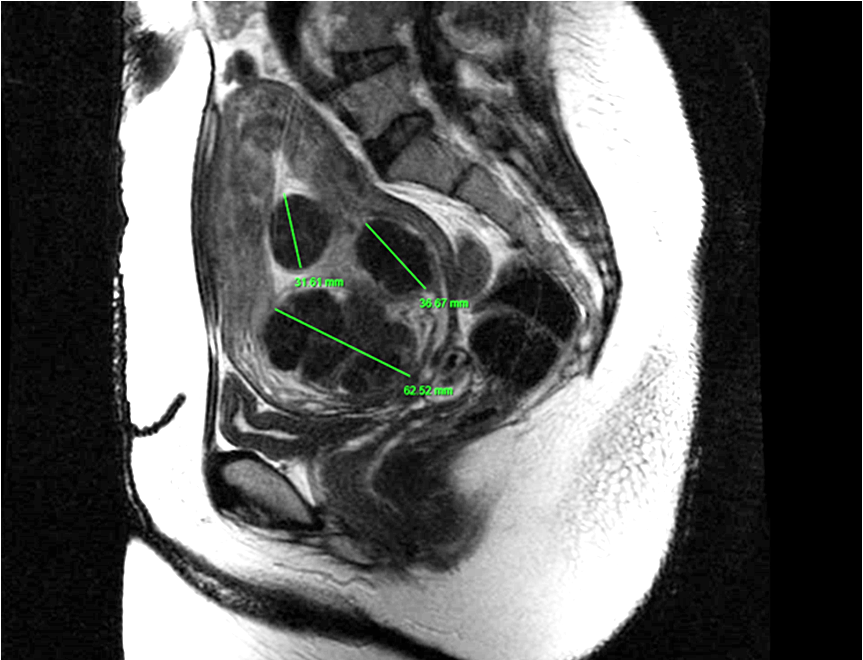
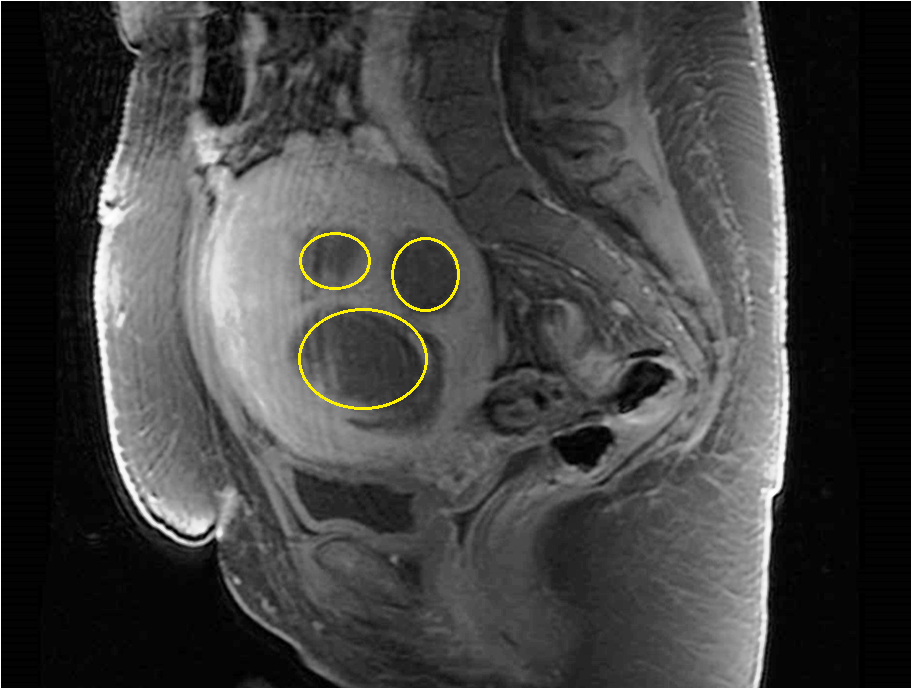
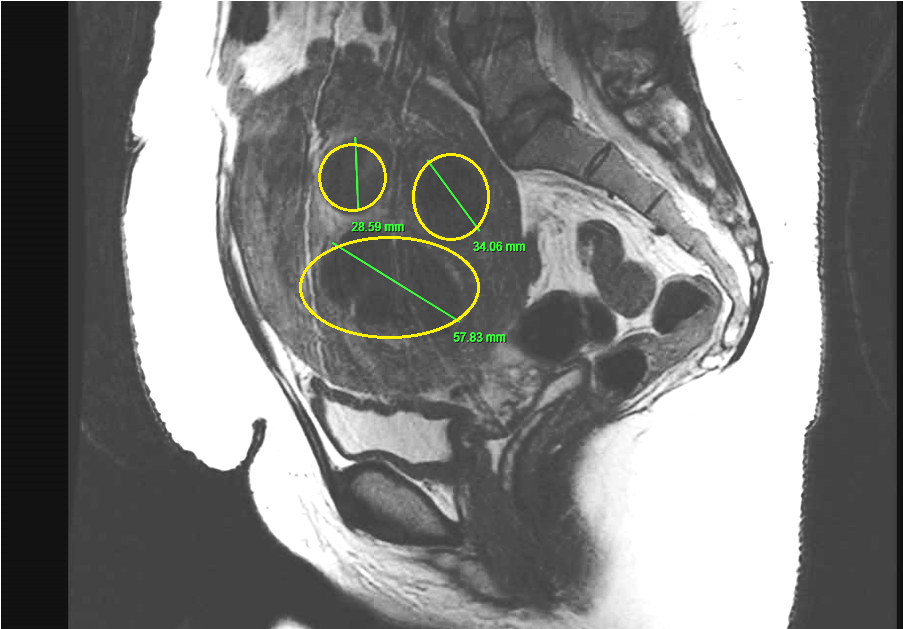
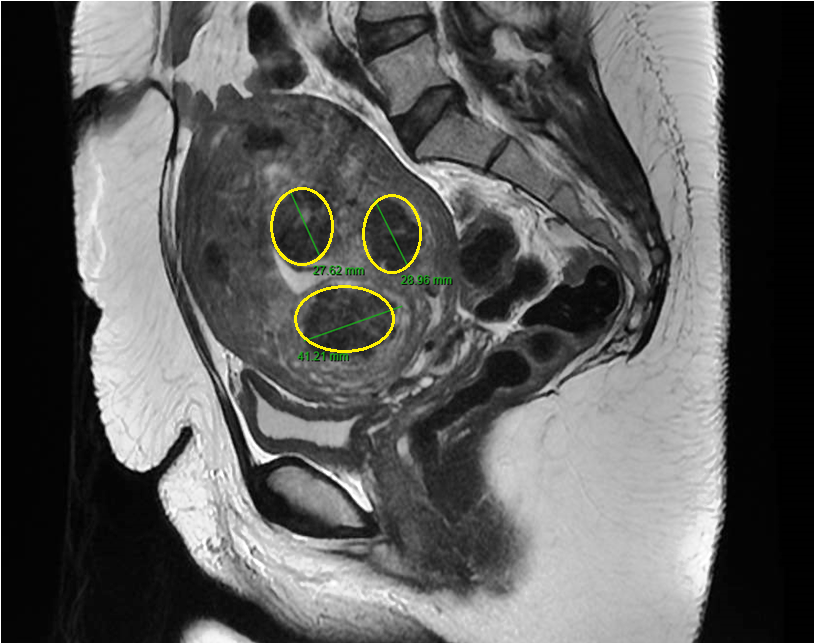
This procedure is also known as Transcervical Radio Frequency Ablation of Myoma (TRFAM). It uses radiofrequency energy to ablate uterine fibroids, under intrauterine ultrasound guidance, resulting in coagulative necrosis of the fibroids. In simple English, radiofrequency applies electromagnetic waves with rising temperature to the fibroid(s). This heat energy causes the fibroids to shrink in size and consequently they become inactive.
It is a recently developed method and carried out by gynaecologist. In UK, this procedure using the SONATA system is, as of June 2020, available only at St. Marys Hospital, London.
Key features includes:
| Suitable types of fibroids | Submucosal, intramural and transmural fibroids. Up to 6 cm. |
| Unsuitable types of fibroids | Extramural (e.g. cervical, broad ligament) and pedunculated fibroids. |
| Uterus preservation. | Yes. Only fibroids are removed. The womb is left intact. |
| Fertility preservation. | Yes. |
| Surgical cut? | Incesionless (i.e. No surgical cuts, no scars) |
| Anaesthesia. | Alone or in combination: general, regional and/or conscious sedation. |
| Operation time | Average total just under 40 minutes (38.8 ± 22.5 minutes), depending on the number of fibroids and size of each fibroid. One ablation will require 2-7 minutes. |
| How soon to return to normal activity? | On average, 4.4 days. |
In addition, this technique is claimed to offer:
- To avoid the risks of laparoscopic (keyhole) or open myomectomy/
- the fertility-effecting problems sometimes encountered with uterine artery embolisation (UAE).
- as alternative where MRgFUS is restricted.
- as an option in recurrence of fibroid where the patient has previously undergone open myomectomy.
What are the complications of this procedure?
Known complications include:
- Increased vaginal discharge: 14.5% to 15.2%.
- Reoperation: 4.3% to 8%
- Hysteroscopic resection of intracavity free myoma: 0.97%.
What to expect BEFORE the procedure?
Some tests are being carried out to make sure that you are fit for the procedure which include:
- Physical examination.
- Pregnancy test.
- MRI scan.
- Check what medications you are taking regularly.
- Check your blood levels for haemoglobin to see if you are fit enough to go ahead.
- Check blood pressure, heart rate and ECG to see if the heart is fit.
- Possibly chest x-rays.
What happens ON THE DAY and BEFORE the operation?
- You will be taken to a waiting room where a nurse will check you in. You will be seen by gynaecologist who will ask the date of your last menstrual period. You will also have the procedure explained to you and be asked to sign a written consent form.
- One hour before the operation, you will be given an anti-inflammatory & pain killers as well as anti-sickness/nausea medications. Also to soften the cervix to make resectoscope entry easier, you may be given medications to insert into the vagina.
- An anaesthetist will meet you to go though the type of anaesthesia applicable for your case and ask questions on previous operation(s) (if you've had any and also your family).
- If you choose to have GA, in the pre-op room, an intravenous line is inserted for drugs to be given. Then next 2 steps are applicable to you.
- You will be moved to the operating theatre where various monitors will be connected to help to care for you while you are anaesthetised.
- The anaesthetist will put you to sleep. Tube may be put into your mouth to help you to breathe and taken out at the end of the operation. She/he will stay with you throughout the surgery to make sure that you remain safe throughout.
What happens DURING the procedure?
Please, watch the animated video below to get an idea what entails.
Essentially, the procedure involves:
- 1. Under anaesthetics, the surgeon inserted the "hand piece" through your cervix to locate and target each fibroid.
- 2. With the use of guided ultrasound, location and size are determined to provide suitable ablation zone and temperature.
- 3. Introducer and then Needle Electrodes are deployed into the fibroid to which radio frequency waves are applied to burn off the fibroid for a duration of 2-7 minutes.
- 4.Step 3 is then repeated as required.
What happens AFTER surgery?
- You will be moved to the recovery room to be cared for by a specialist nurse until you are stable and then transferred to the ward. Generally, you are being monitored for 2-3 hours.
- You may have some cramping abdominal pains and pain relief is given for this.
- Some vaginal blood loss may occur but not too much to cause concern.
- Once you are fully recovered, you will be given a drink and a light meal.
- You are ready to go home as soon as you are awake, tolerate fluid & food without undue pain.
- Take home medications include NSAID anti-inflammatory drug(s) and antibiotics to prevent infection of necrotic (dying) fibroid tissue.
Care afterwards...
Your self-care guide involves performing activities that aid your recovery.
- You may feel drowsy in the first 24 hours and it is advisable that you do not drive or operate machinery.
- You may experience cramping symptoms. If this is the case, you can take paracetamol (e.g. Panadol) or ibuprofen such as Nurofen (only if you are not allergic to it, or asthmatic or have history of stomach ulcers). If you are in doubt, ask your pharmacist.
- Rest for a couple of days then gradually resume your normal activities.
- You may get vaginal bleeding lasting 2-4 weeks and it should settle after that. Do not use tampons, only use sanitary towels.
- You may still see a pinkish/brown/yellow or clear vaginal discharge in the first 2-4 weeks which is common as the womb heals.
- Don't use tampons until the blood stained discharge has stopped as this could introduce infection.
- Use the shower instead of the bath in the first 2 weeks.
- You can have sex again as soon as the discharge stops. Do continue contraception as before, unless you are wanting to get pregnant.
- Depending on your speed of recovery, you can go back to work and continue with normal activities within about one week.
When should I seek emergency medical attention?
While it is unusual to have problems once you are at home, seek immediate medical attention if any of the following occurs:
- Fever with temperature above 38℃ or chills.
- Headache/dizziness.
- Increased abdominal pain which is not relieved by pain medications.
- Increased/prolonged bleeding.
- Unusual foul-smelling vaginal discharge (yellow/green colour).
- Discharge from wound or wound opening.
- Frequent urination or burning sensation when passing urine.
- Difficulty or unable to pass urine.
Follow up...
The hospital will arrange for a follow-up appointment in 3 months, with MRI scan to assess the result of the operation.
Acknowledgements
BFT thanks: (i) Mr Stephen D. Quinn MSc MD MRCOG,Consultant Obstetrician and Gynaecologist, St Mary’s Hospital, London UK; for his input. (ii) Gynesonics for their provision of the animated video.
Last updated on Monday 1 February 2021 11:57 am.
Related Topics
Jargon Buster
Fibroids FAQs
Adhesion & Asherman's Syndrome
Fibroids & Intertility
Fibroids & Cancer
MRI scans of RFAUF